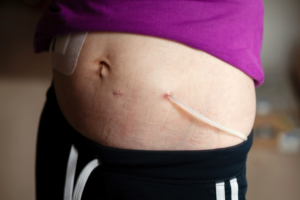
Peritoneal Dialysis
Contents:
Benefits and Challenges
Benefits:
- Less travel expenses than in-center treatments
- Potential for higher care satisfaction compared to in-center treatments1
- Choosing PD more closely mimics the natural action of your kidneys and is done more consistently than hemodialysis, which can lead to better health outcomes2
- Increased flexibility since treatments are either done as you sleep or can be completed at work and at your convenience
- Less dietary restrictions than hemodialysis
- You don’t need a needle to engage in treatment
- Being at home means that you don’t need to be around other patients that could be sick
- More flexibility to travel as compared to in-center dialysis
- Your blood stays in your body and does not go through a machine
- Works for patients that are not strong candidates for a fistula or an arterio-venous graft
Drawbacks:
- You do need substantial space to perform exchanges and to store supplies
- Catheters run a higher risk of infection (peritonitis), especially if they are not well maintained3
- Unless precautions are made, you can’t take a bath above your waste or swim
- More control over the therapy does mean you are more involved and there are no full off-days
- Depending on the type of treatment, you might have to dwell during the day and this can make you feel bloated or impact your appearance
- The dialysate solution contains sugar, which can lead to weight gain if not closely monitored
- Due to dextrose used in the dialysate, diabetic patients might have trouble managing their disease. However, new substances are being used that have little impact on blood sugar levels4
- Some patients also will need a dedicated caregiver or partner to help in exchanges or supply management
- Risk of changes to the peritoneum may cause patients to need to switch to hemodialysis
- Risk of back strain, hernias and muscle injuries caused by extra abdominal weight and pressure5
- Potential for a decrease in lean body mass and protein loss during treatments.6
1. Rubin Haya R., Fink Nancy E., Plantigna Laura C., et al. Patient Ratings of Dialysis Care with Peritoneal Dialysis vs Hemodialysis. Journal of the American Medical Association. 2004; 291(6): 697-703. Retrieved from http://jama.jamanetwork.com/article.aspx?articleid=198181#qundefined.
2. Chertow GM., Levin NW., Beck GJ., et al. In-Center hemodialysis six times per week versus three times per week. New England Journal of Medicine. 2011 Jan 6;364(1):93. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/21091062.
3. Lafrance Jean-Philippe, Rahme Elham, Iqbal Sameena, et al. Association of Dialsis Modality with Risk for Infection-Related Hospitalization: A propensity Score-Matched Cohort Analysis. Clinical Journal of the American Society of Nephrology. 2012. Published online at http://cjasn.asnjournals.org/content/early/2012/08/15/CJN.00440112.full.
4. Dasgupta Mrinal K., Management of Patients with Type 2 Diabetes on Peritoneal Dialysis. Advances in Peritoneal Dialysis. 2005 Vol 21. Retrieved from http://www.advancesinpd.com/adv05/Adv20053d-1.pdf.
5. Mahale AS., Katyal A., Khanna R., Complication of peritoneal dialysis related to increased intra-abdominal pressure. Advances in Peritoneal Dialysis. 2003; 19:130-5. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/14763049.
6. Stenvinkel Peter, Lindholm Bengt, Lonnqvist Fredrik., Increases in serum leptin levels during peritoneal dialysis are associated with inflammation and a decrease in lean body mass. Journal of the American Society of Nephrology. 2000 Vol 11:7 1303-1309. Retrieved from http://jasn.asnjournals.org/content/11/7/1303.full.