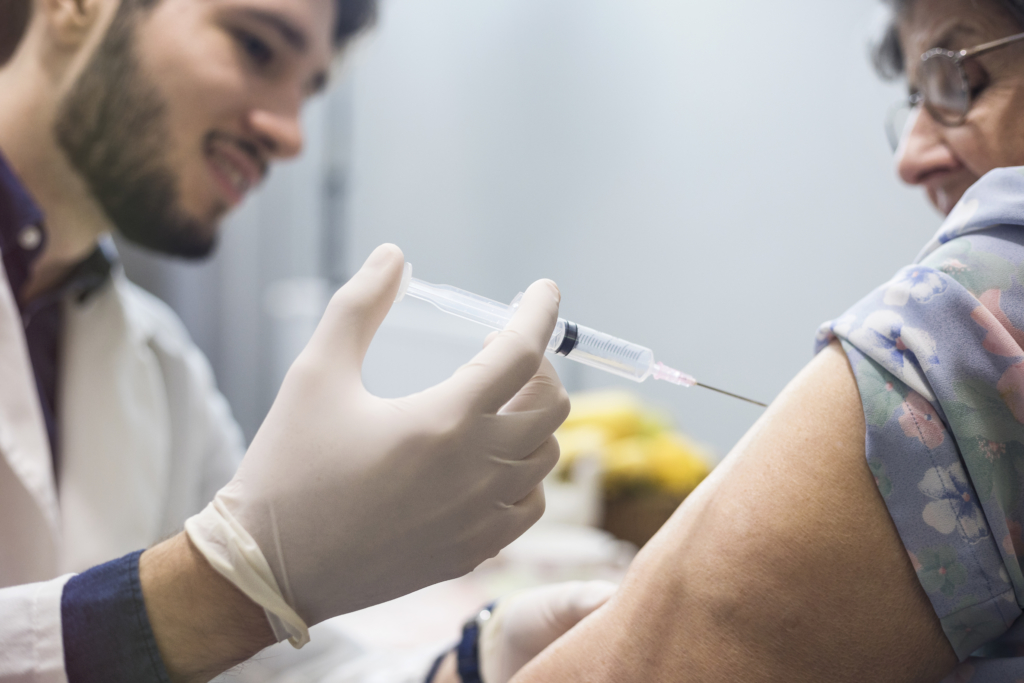
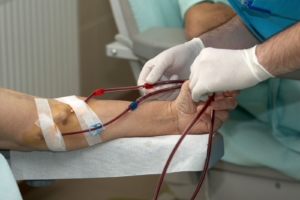
Treatment
Although there is no cure for kidney disease, learn what you can do if you have Stage 5, End-Stage Renal Disease (ESRD). You have a number of treatment options to consider as you determine with your health care team which one works best for your life style.
Contents:
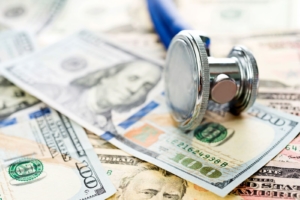
Treatment for kidney failure is costly. Whether you choose dialysis or a transplant, insurance coverage is essential to cover the cost of these treatments. Once you are diagnosed with kidney failure, you may be eligible to receive Medicare coverage regardless of your age. You can learn more in the Medicare Coverage of Kidney Dialysis & Kidney Transplant Services booklet.
In the following sections we will provide a brief overview of the various insurance options available to you as a dialysis patient.
According to the United States Census Bureau’s Health Insurance Coverage in the United States:2019 report, 92 percent of people had health insurance coverage at some point during the year. Of those, 68 percent had private health insurance.
The Social Security Act assures that patients who are diagnosed with ESRD and have private insurance can keep their plan for up to 30 months. After that time, Medicare becomes the primary payer for health services and the private plan becomes the secondary payer. To find the best coverage option, it is suggested you speak with your insurance provider or your dialysis social worker.
The health insurance exchange plans were established by the Affordable Care Act and first became available in 2013. Patients who do not have coverage through employment, Medicare or Medicaid can enroll in an exchange plan. During the open enrollment period every year, different types of exchange plans are available for purchase. This can be done online, by phone, by mail or in person.
The amount of coverage an exchange plan provides depends on the type of plan purchased. Some exchange plans can have narrow networks, limiting the amount of nephrologists, hospitals and dialysis clinics available to an ESRD patient. Research is recommended to determine the suitable type of plan for a patient.
Some states operate their own exchange, while others use the federal marketplace. To find out what type of exchange is offered by your state, visit our state resources page.
Medicare is government-provided health insurance for:
- People who are 65 years of age and older
- People under 65 years of age with certain disabilities
- People of any age who are diagnosed with End-Stage Renal Disease (permanent kidney failure requiring dialysis or kidney transplant) and meet certain requirements.
To be eligible for Medicare when diagnosed with ESRD, one of these must apply to you:
- You have worked the required amount of time under Social Security (SS), the Railroad Retirement Board (RRB), or as a government employee.
- You already receive or are eligible for SS or RRB benefits.
- You are the spouse or dependent child of a person who meets either of the above requirements.
Under Medicare, End-Stage Renal Disease (ESRD) patients can sign up for Original Medicare or Medicare Advantage.
With original Medicare, you can go to any doctor or provider that accepts Medicare and is accepting new patients. ESRD patients will need Part A, Part B, and usually Part D to get all the benefits available to them.
Medicare Part A does not usually require a monthly premium. Part A Covers:
- Inpatient hospital care
- Inpatient care in skilled nursing facilities, hospice, and some home health care
There is a monthly premium for Medicare Part B. After you pay a yearly deductible, Medicare will pay 80 percent of your monthly costs and you will be responsible for paying the remaining 20 percent. If you have a secondary form of insurance, it can cover these additional costs. Part B Covers:
- Doctor’s services, outpatient care including dialysis treatments, and home health care.
- Some preventive services to help maintain health and to keep certain illnesses from getting worse.
Medicare Part B will cover most of the drugs you may need during your dialysis treatment. However, it will not cover the medications you need to get through your pharmacy including prescriptions for other health conditions such as high blood pressure, high cholesterol, or diabetes. These drugs can be covered by Medicare Part D, which is offered by private insurance companies approved by Medicare and requires a monthly premium in addition to Part B payment. Some dialysis facilities and corporations have their own pharmacy where you can buy your medications.
Medicare Advantage
Medicare Part C is referred to as a Medicare Advantage Plan. Medicare Advantage plans are health care plans offered by private insurance companies that provide extra benefits and coverage.
With a Medicare Advantage Plan or ‘MA’ Plan, you use a health insurance card and may be restricted to see certain doctors or hospitals that are a part of your plan. MA Plans include:
- Medicare Health Maintenance Organizations (HMOs)
- Preferred Provider Organizations (PPO)
- Private Fee-for-Service Plans
- Medicare Special Needs Plans
ESRD patients are only eligible for Medicare Advantage if:
- You’re already in a Medicare Advantage Plan when you develop ESRD. You may be able to stay in your plan or join another plan offered by the same company.
- You’re already getting your health benefits (for example, through an employer health plan) through the same organization that offers the Medicare Advantage Plan.
- You had ESRD, but have had a successful kidney transplant, and you still qualify for Medicare benefits (based on your age or a disability). You can stay in Original Medicare, or join a Medicare Advantage Plan.
- You may be able to join a Medicare Special Needs Plan (SNP) for people with ESRD if one is available in your area.
You have a one-time right to join another MA plan if both of the following are true:
- You have ESRD and are in a Medicare Advantage Plan
- The plan leaves Medicare or no longer provides coverage in your area. You don’t have to use your one-time right to join a new plan immediately.
If you are interested in joining a MA Plan or have questions, you can contact the state health insurance assistance program, Medicare.gov, or call Medicare at 1(800) 633-4227.
Medigap
Medigap is a supplemental insurance policy that is designed to cover health care costs that Medicare doesn’t cover. This means Medigap insurance will cover the additional 20 percent costs that Medicare does not pay, such as co-pays or deductibles. You must have Original Medicare Part A and B to purchase a Medigap Policy, and Medigap policies require a monthly premium in addition to Part B.
Unfortunately, Medigap is not currently available to all dialysis patients. It is available to all patients over the age of 65, but only available to those under 65 in 28 states. Find out if your state offers Medigap coverage.
Medicaid
Medicaid is a state program that is available to those with low income and/or resources. Some people who have Medicare use Medicaid a secondary insurance to cover the 20 percent that Medicare does not. If a patient doesn’t qualify for Medicare, Medicaid can be used as the only coverage.
As every state has its own Medicaid coverage, the state determines:
– Eligibility Guidelines
– Services Covered
– Payment Rate
To find out about your state’s Medicaid program, contact your state’s department of health or speak to your social worker or insurance coordinator at your facility.
Learn More About Treatment

Treatment
Chronic kidney disease may progress to End-Stage Renal Disease, which has a number of treatment options.

Early Intervention
There are proactive actions you can take to decrease your chances of developing kidney disease in the future.

Medication
It is important to take all of your medicines as prescribed for your kidney disease, even if you don’t notice an immediate difference.