By Alan Kliger, MD
Updated March 18, 2022
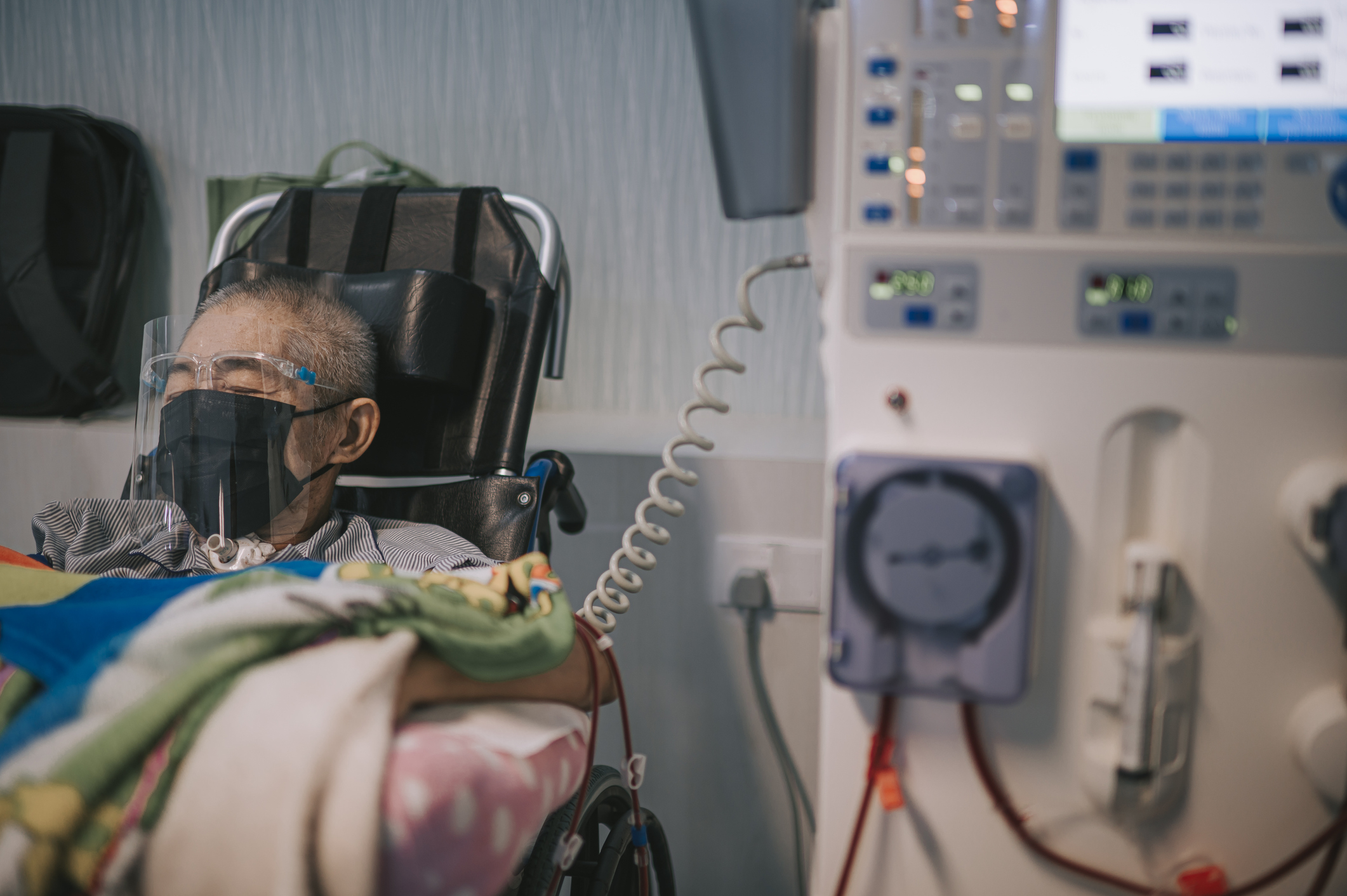
I am writing this mid-March 2022, as the last peak of COVID infection with the Omicron variant has rapidly fallen in every US state, but wastewater analysis has shown places in the US where virus infection in some communities is rising again. A new sub-variant, BA.2 is making up about 23% of cases. Abroad, the United Kingdom is seeing increasing hospitalizations with COVID infection, and many locations in the far east have raging infections. The effects of the surge in Omicron cases around the world this past winter have deeply affected patients on dialysis … effects likely to last well into the spring of 2022, even if we see no further surges or new variants of this wily virus. The pandemic’s effect on our healthcare system and on the dialysis industry are widespread, causing supply shortages, supply chain disruptions, and personnel challenges, including the “Great Resignation” where roughly 33 million Americans have quit their jobs since the spring of 2021. Remaining workers have experienced stress, overwork, and burnout. Disagreements about use of face masks, vaccines, and government mandates fracture the country and engender mistrust and anger. Dialysis facilities reflect many of these stressors and have made adjustments to try to keep patients safe. Here is a partial list of these effects of this two-year pandemic:
The Great Resignation
- Nursing and dialysis technician staff shortages have occurred across the country. As many as 1 in 4 or 1 in 5
 staff have left their jobs, part of the “Great Resignation.” Retention bonuses have had limited utility in keeping many professional caretakers at their jobs. Attracting new staff to work in the vacancies has proven very difficult, even when monetary incentives are offered such as signing bonuses. These staffing shortages have in some areas resulted in shift closures, and even facility closures. Other facilities have considered reducing dialysis time, to allow reduced staff caregivers to deliver dialysis to all patients.
staff have left their jobs, part of the “Great Resignation.” Retention bonuses have had limited utility in keeping many professional caretakers at their jobs. Attracting new staff to work in the vacancies has proven very difficult, even when monetary incentives are offered such as signing bonuses. These staffing shortages have in some areas resulted in shift closures, and even facility closures. Other facilities have considered reducing dialysis time, to allow reduced staff caregivers to deliver dialysis to all patients. - Fewer staff caring for more patients (in those shifts that remain open) are spending all of their time in direct patient care, leaving little or no time for activities such as quality improvement, patient-centered projects, or data collection and reporting. At such stressful times, it is difficult for facilities to compile government-mandated data and report these data, which in turn will make it difficult to use data to understand our quality and safety challenges.
- Disruptions in manufacturing and supply chain have caused shortage of some dialysate solutions. Even when manufacturers are able to produce these essential solutions, truck drivers and delivery personnel shortages reduce the numbers of these supplies that are delivered on time, as needed to dialysis facilities across the US. The result is that many dialysis facilities have reduced the volume of dialysate for each dialysis. For example, in facilities where a standard dialysate flow rate is 800ml/min., these rates have been reduced to 600 or 500 ml/min to preserve available dialysate solution and assure the supply for all patients. While studies have shown that the effectiveness of dialysis at these slower dialysate flow rates in not reduced very much, these slower dialysate flow rates are somewhat less than ideal. Manufacturers have had reduced plant inventory of some varieties of dialysate solution, so the solution used by some patients have needed to change. Dialysis staff have carefully monitored patient blood tests and measured the effectiveness of dialysis as measured by Kt/V measurements, to assure that these changes do not result in meaningful changes in patient care.
 Vaccination
Vaccination
Dialysis patients and staff have been strongly encouraged to get COVID-19 immunization and boosters when eligible, and these populations are among the highest percent immunized in most communities. While some have been skeptical and reluctant, many more have sought to get fully immunized and boosted as soon as possible. Some studies have shown that patients who are immune-compromised, such as kidney transplant patients taking immunosuppressive medicines, have a much lower response to COVID-19 vaccine than the normal population. The lower levels of antibody that these patients develop in response to immunization makes these patients more susceptible to COVID-19 infection and its complications. Some studies have shown that patients with chronic kidney disease on dialysis, many of whom have other system diseases such as diabetes, hypertension, heart, and vascular disease, also have reduced antibody production after vaccination. It is difficult to identify which dialysis patients are immune-compromised and which are not. For this reason, many nephrologists believe it is prudent to identify all dialysis patients as immune-compromised, and to offer them the same protection as the CDC recommends for moderately or severely immune-compromised individuals. That includes an extra dose of mRNA or vector vaccine to be considered fully vaccinated, and then booster doses after 3 – 6 months.
Treating COVID-19 Infection
Until recently, there was little that patients with mild or moderate COVID-19 infection could do other than rest, isolate, take pain medicine as needed, and stay well-hydrated. There were no effective anti-viral medicines similar to antibiotics that treat bacterial infections like staph. In recent months, FDA has given emergency use authorization to several drugs and drug combinations that effectively reduce the viral load and decrease the symptoms and possible complications of COVID-19. Remdesivir, which has been used in hospitals to treat severe COVID-19 infections, now is available for outpatients and works well against this virus. However, it has not been studied adequately in patients with kidney disease and is not currently advised for dialysis patients. Other new ant-viral medicines have come on the market, but also have not been approved for use in dialysis patients. Paxlovid is a combination medication that works well to treat Omicron but has several drug interactions that limits its use. It has not been approved for use in patient with advanced kidney disease or dialysis. These and other anti-viral medicines need to be studied more carefully in patients with advanced kidney disease before they can be widely used.
Another category of medicine, monoclonal antibodies, have been used to reduce disease complications and even can be used prophylactically to prevent infection in patients at risk. Sotrovimab is an engineered neutralizing monoclonal antibody that unlike earlier developed monoclonal antibodies, shows strong evidence of stopping spread of the Omicron variant. Evushield, a combination of 2 long-acting human monoclonal antibodies, has been authorized for COVID-19 prophylaxis in patients at high risk for this infection. Dialysis patients, considered by many nephrologists as immune-compromised and at high risk of infection, are therefore candidates for this therapy.
In summary, while the Omicron Variant of COVID-19 is rapidly receding, new waves of infection remain possible. The effect of a two-year pandemic on the workforce, including dialysis personnel, has had profound effects on our ability to provide routine dialysis across the US. Fewer nurses and technicians, fewer drivers and supply delivery personnel have together reduced the number of dialysis stations operating across the country and have limited availability of dialysis solutions. While safety remains the top priority of dialysis providers, these limitations have substantially stressed the dialysis industry. COVID vaccination and boosters have proven very successful in reducing illness and death in the dialysis population: before these therapies were available, dialysis patients infected with COVID-19 often had a 20% or higher death rate. Since most patients have been immunized, the mortality and hospitalization rate for COVID-19 sufferers on dialysis is far lower. New anti-viral medications and monoclonal antibodies are effective in treating non-hospitalized COVID-19 patients, and we need more study on the safety and efficacy of these medications in dialysis patients. A long-acting monoclonal antibody combination Evushield has been useful to prevent infection in high-risk patients with immune-deficiency and may prove valuable for the dialysis population.
Alan S. Kliger, MD, Clinical Professor of Medicine, Yale School of Medicine, and Chair, Excellence in Patient Care Advisory Committee, American Society of Nephrology